Two divers complete the same dive on the same day — same depth, same bottom time, same ascent rate, same surface interval. One surfaces fine. The other develops decompression sickness. It is a scenario that plays out in hyperbaric chambers around the world every year, and one that has never been fully explained by standard dive medicine.
A new research initiative based in the Red Sea is now taking direct aim at that question — and the answers it uncovers could change how the global diving community understands, plans, and manages individual decompression risk.
The Study and Who Is Behind It
The project is led jointly by Hypermed Red Sea and Baromedical Red Sea, with operational support from Emperor Divers, whose liveaboard fleet operates throughout the Egyptian Red Sea. The medical team is headed by Dr Hossam Nassef and Dr Hanaa M Nessim, with field operations coordinated by Dr Abdelrahman Hossam and Dr Abdelhakim Hossam.
Rather than focusing on the dive profile — depth, time, ascent rate — the study shifts its primary lens to the individual diver. The underlying premise is straightforward but underexplored in applied dive medicine: physiological variation between divers may be just as significant a risk factor as any element of the dive itself.
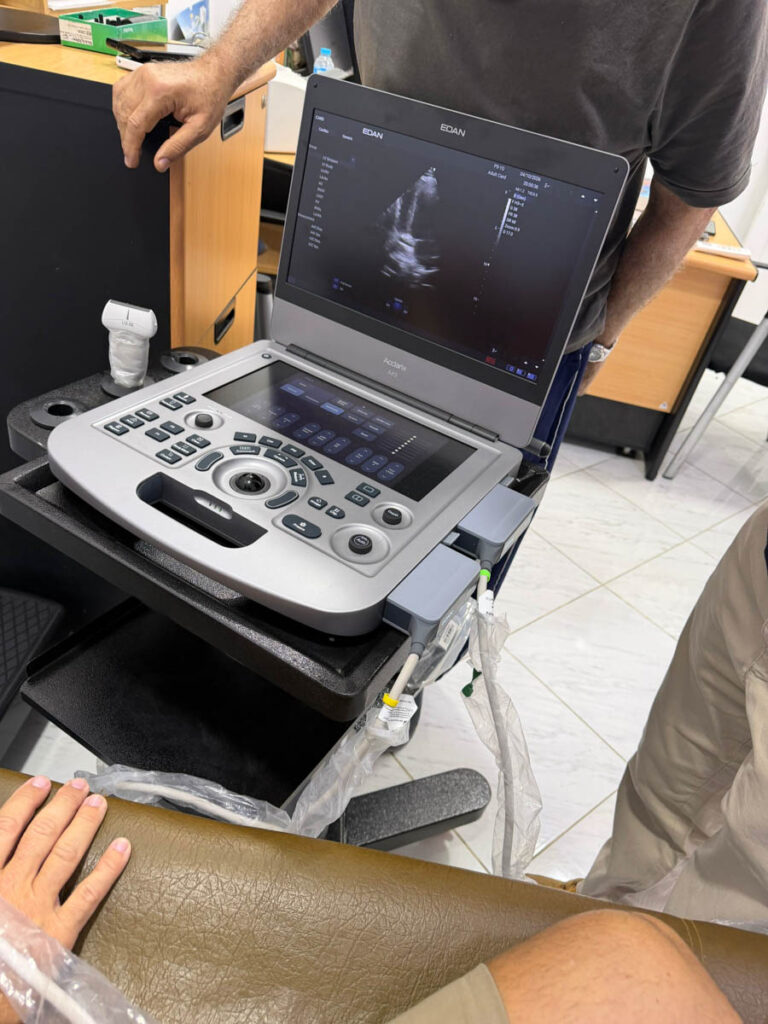
At the core of the methodology is Doppler ultrasound technology, a diagnostic tool capable of detecting microbubble formation in the bloodstream after a dive. These microbubbles — silent, invisible, and often symptom-free — are a known indicator of decompression stress. The ability to measure them with precision, in real-world diving conditions rather than laboratory simulations, is what makes this study significant.
The Science Behind the Question
Under pressure at depth, nitrogen dissolves into body tissues. As a diver ascends and ambient pressure decreases, that nitrogen comes back out of solution. Managed correctly — with gradual ascents and safety stops — the gas is eliminated through the lungs without incident. But when the process is disrupted, or when individual physiology does not respond as the decompression models predict, bubbles can form in the tissues and bloodstream, causing decompression illness ranging from joint pain and skin rashes to neurological damage and, in severe cases, death.
What the standard models do not fully account for is individual variation. Two divers with the same certification, fitness level, and dive experience can have measurably different bubble loads after an identical dive. Factors such as body composition, hydration, cardiovascular health, patent foramen ovale (PFO) — a common heart defect in which a small opening between the heart’s upper chambers fails to close after birth — and even genetics are all believed to play a role. But the precise contribution of each factor, and how they interact, remains poorly understood.
This study aims to begin filling that gap. By comparing divers with matched profiles — similar age, sex, body composition, and dive history — and tracking their post-dive bubble loads using Doppler monitoring, the research team hopes to identify the physiological variables that correlate most strongly with elevated decompression stress, even in the absence of symptoms.
Why the Red Sea Is the Right Place for This Research
The Red Sea is not simply a convenient backdrop for this study — it is arguably the most appropriate dive environment on the planet for this kind of research. Egypt’s Red Sea coast, and Hurghada in particular, hosts one of the highest concentrations of recreational and technical diving activity anywhere in the world. Thousands of dives are conducted here daily, across a wide spectrum of profiles, diver backgrounds, and certification levels.
That volume of diving activity, combined with an established medical infrastructure that includes hyperbaric facilities experienced in managing dive-related injuries, creates a rare research environment. Real-world data, gathered in real conditions, from a genuinely diverse population of active divers — this is precisely what previous decompression research has often lacked.
As Dr Nassef explained when discussing the rationale behind the project: in daily clinical practice, the medical team routinely encounters divers who have developed decompression illness despite following their computers and dive plans to the letter, while others make similar or deeper dives without consequence. Moving from clinical observation to measurable physiological data is the study’s central objective.
What the Findings Could Mean for Divers
The practical implications of this research extend well beyond academic diving medicine. If the study can identify reliable physiological markers of elevated decompression risk, the impact on how divers are assessed, trained, and supported could be significant.
For recreational divers, the findings could eventually inform pre-dive medical screening protocols, helping identify individuals who may need to modify their dive profiles or seek further cardiovascular assessment before diving regularly. PFO, for example, is estimated to be present in roughly one in four people — many of whom dive without ever knowing it — and is associated with a higher risk of decompression illness under certain conditions. Earlier identification could prevent serious injury.
For technical divers, where decompression obligations are longer, deeper, and more complex, personalised decompression strategies informed by individual bubble load data could offer a meaningful safety improvement over the current one-size-fits-all table and computer models.
The Doppler equipment used in the study has been funded entirely through contributions from Emperor Divers and its guests — a reminder that advances in diving safety are often driven not by government agencies or pharmaceutical investment, but by the diving community itself, quietly pooling resources around problems that matter.
Emergency Response Running in Parallel
Alongside the Doppler research, the team is also expanding an emergency awareness programme in collaboration with Red Sea Lifeboat Medevac, focused on improving response times and raising diver and operator awareness around the early recognition and management of decompression illness and other diving-related injuries. Rapid response in the critical window following symptom onset remains one of the most important variables in diver outcomes — and awareness, at every level of the industry, is the foundation of that response.
A Shift in How We Think About Diver Safety
For too long, the conversation around decompression safety has been dominated by dive computers, tables, and ascent rates — all of which are essential, but none of which tell the complete story. The human body is not a uniform system, and decompression models built on population averages will always carry limitations when applied to individuals who sit outside those averages.
This Red Sea initiative represents a meaningful step toward a more personalised, data-driven approach to diver safety — one that treats the diver, not just the dive, as a critical variable. That is a shift the entire industry should be watching closely.
Mohsen Nabil is the Founder and Editor-in-Chief of Diventures Magazine. A mechanical engineer and scuba diving instructor based in the Red Sea, he writes about diving safety, marine conservation, underwater exploration, and developments in the global dive industry. Through Diventures Magazine, he works to connect divers, scientists, and ocean advocates while promoting responsible diving and protection of the oceans.







